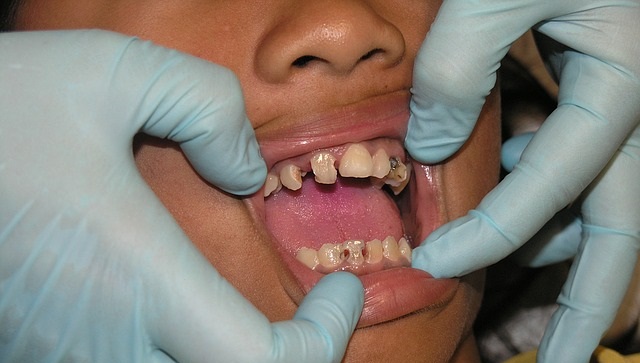
If you are concerned about dementia or getting Alzheimer’s disease then you might want to take better care of your teeth. A new study published in Alzheimer’s & Dementia: Diagnosis, Assessment & Disease Monitoring (DADM) shows a link between gum disease and a loss of cognitive abilities later in life.
DADM is an open access journal that concentrates on the discovery, development, and validation of assays, instruments, and technologies with the potential to facilitate accurate detection of dementia in its various forms and stages.
Will you offer us a hand? Every gift, regardless of size, fuels our future.
Your critical contribution enables us to maintain our independence from shareholders or wealthy owners, allowing us to keep up reporting without bias. It means we can continue to make Jewish Business News available to everyone.
You can support us for as little as $1 via PayPal at office@jewishbusinessnews.com.
Thank you.
Gum disease is caused by the proliferation of bacteria in the mouth. The bacteria basically eat away at your gums. The gums recede leaving more of the teeth exposed. This is called periodontal disease. Proper oral hygiene, brushing one’s teeth regularly and using mouthwash, can prevent this. So can the regular use of dental floss.
Poor oral hygiene is the reason why so many people end up needing extensive dental work later in life. This includes the use of dentures. And now it may also lead mental degradation such as dementia. But there is also healthy bacteria. And the presence of such bacteria might help to prevent dementia. But this bacteria loses out in competition with the unhealthy kind which causes gum disease.
The study’s authors say that as far as they know this is the first report of an association between subgingival periodontal bacteria and CSF biomarkers of AD pathology in cognitively normal elderly people. They found that subgingival periodontal dysbiosis characterized by increases in periodontal‐associated bacteria and decreases in health‐related bacteria associated with reduced CSF Aβ42 but not with CSF P‐tau.
Periodontal disease (PerioD) is an oral, chronic, inflammatory, dysbiotic bacterial condition affecting more than 50% of elderly people. Up to 700 species colonize the subgingival biofilm; among them, several known periodontal bacterial species are enriched in PerioD, including: Porphyromonas gingivalis, Tannerella forsythia, Treponema denticola, Prevotella spp, Porphyromonas endodontalis, and Fretibacterium fastidiosum.
The researchers point out that it is well known that periodontal bacteria, particularly in the presence of oral inflammation, gain access to the systemic circulation and can impact distant sites including heart, joints, and liver. Some forms of periodontal bacteria are also associated with cancer. Recent evidence suggests that the brain can also be affected.
Dr Angela Kamer from the New York University College of Dentistry and the study’s lead author explained that “The mouth is home to both harmful bacteria that promote inflammation and healthy, protective bacteria. We found that having evidence for brain amyloid was associated with increased harmful and decreased beneficial bacteria. Our results show the importance of the overall oral microbiome – not only of the role of ‘bad’ bacteria, but also ‘good’ bacteria – in modulating amyloid levels.”